There are 1,627 cases of monkeypox in Mexico
As of September 26, the Mexican Ministry of Health had confirmed 1,627 cases of monkeypox across the country, with 967 of those cases occurring in Mexico City alone.
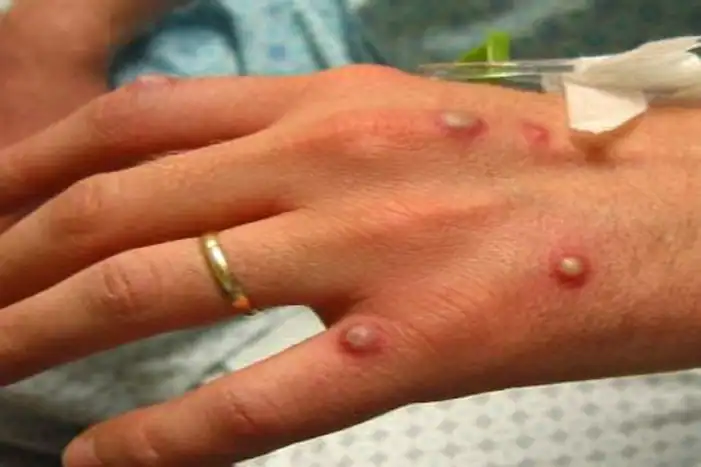
As of September 26, the Mexican Ministry of Health had confirmed 1,627 cases of monkeypox across the country, with 967 of those cases occurring in Mexico City alone.


Mexico's archery team shines at Paris 2024 Olympics. The women's team secures third place, advancing to the quarterfinals. Alejandra Valencia leads with a strong performance. The men's team qualifies for round of 16. Matías Grande and Valencia aim for mixed team podium.

Mexican lawmakers propose tax incentives for foreign film productions. The goal is to boost the local film industry, create jobs, and attract international investment. The initiative offers tax certificates to foreign investors, which can be transferred to Mexican companies.

Representative Gabriela Sodi (PRD) proposes reforming Article 21 of Mexico's Constitution to establish autonomous, independent, and professional expert services to provide scientific data for criminal investigations.

Mexico faces a blood shortage due to low voluntary donors. Only 5% donate altruistically. Dr. Contreras Serratos urges people to donate blood regularly, starting at 18. Donating blood is safe and helps others in need.